Osteoporosis is a condition that results in reduction of bone strength (density), leading to increased risk of fractures.
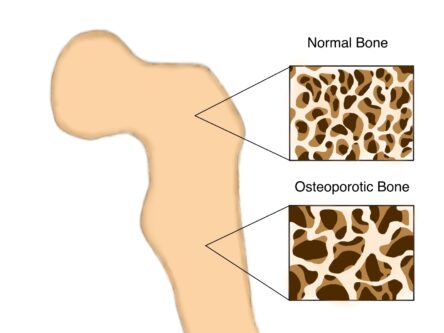
Bone strength is determined by the structure and the mineral components. Bones are formed of a mineral called calcium hydroxyapatite with collagen fibers. Bone structure consists of a hard outer shell, called cortical bone and spongy interior called trabecular bone. Bone is constantly being remodeled; older bone is being broken down by cells called osteoclasts, and then rebuilt by cells called osteoblasts.
As we grow up, more bone is built than destroyed, leading to peak bone density around the age of 25. After the age of 40, bone density naturally starts to fall due to increased bone break down. If this is accelerated then the bones can become more fragile and result in osteoporosis.
Osteoporosis is more common with age. In particular females are 4 times more likely to develop osteoporosis. This is due to females having a lower bone density peak than males and following the menopause, the reduction in the hormone oestrogen results in more bone breakdown.
More common risk factors for developing osteoporosis:
Usually the first signs of osteoporosis are insufficiency fractures. These are fractures that occur with less force than suspected to break a bone. Most commonly they occur in the hips, spine or wrists. Often fractures in the spine can occur with no injury, these are known as crush fractures. If there are multiple crush fractures in the spine, the spine can become shorter and curved leading to loss of height.
Osteoporosis is usually suspected after an insufficiency
fracture; this is the most common reason to get investigations carried out. However if you have strong risk factors for developing osteoporosis, then investigations can be carried out before possible fractures occur.
Often a scoring system is used to calculate the risk of fractures to see if you should be investigated- the most common score is the FRAX.
Imaging:
Investigations to look for secondary causes:
Osteoporosis prevention:
Osteoporosis treatments:
Versus Arthritis: http://www.versusarthritis.org
Royal Osteoporosis Society: https://theros.org.uk
Dietary Calcium Calculator: https://www.cgem.ed.ac.uk/research/rheumatological/calcium-calculator/