Idiopathic Inflammatory Myopathies
What are Idiopathic Inflammatory Myopathies?
Idiopathic inflammatory myopathies are a group of rare autoimmune muscle disorders. They characteristically involve myositis, meaning inflammation of the muscles (myo = muscle, itis = inflammation). This results in symmetrical proximal muscle weakness (thighs and upper arms). Other areas of the body can be involved, such as the lungs, heart and gut.
The myopathies are grouped into 3 main subgroups:
- Polymyositis (PM) affects many areas of muscles and usually concentrated around the larger muscles, including the shoulders, hips and thighs.
- Dermatomyositis (DM) is myositis that is also associated with skin rashes.
- Inclusion Body Myositis is a rarer myositis where by proteins build up in muscles, these proteins cannot be broken down. It is a myositis that doesn’t respond to the usual treatments.
These conditions are autoimmune conditions. Usually the immune system protects the body against illness and infection using inflammation, however in autoimmune conditions, the immune system produces proteins called autoantibodies that damage normal healthy tissues.
Myositis can also be associated with other autoimmune diseases such as SLE, Sjögren’s Syndrome and systemic sclerosis.
Causes of Idiopathic Inflammatory myopathies
Polymyositis and Dermatomyositis are rare diseases, affecting 2 people out of 100,000. They mostly affect adults (aged 40-50), although children can be affected, this is called Juvenile Dermatomyositis. Males are slightly more commonly affected than females.
The cause of these autoimmune conditions is complex and not fully understood, but a person’s genetic makeup and environmental factors are important. Genetic studies have found subsets of autoantibodies that help determine the symptoms and progression of the disease.
Environmental factors such as certain infections have been associated with self-limiting forms of myositis. Patterns of affected people with myositis suggest that UV light exposure and vitamin D may play a role. Certain medications have been linked to developing myositis, the most commonly recognised group are statins used to treat high cholesterol. Stopping these medications usually results in disease remission.
Symptoms of Idiopathic Inflammatory Myopathies
Common symptoms:
- Muscle weakness
- Large proximal muscles on both sides of the body (symmetrical).
- Typically the muscles of the shoulders, hips and thighs
- Gradual onset (over weeks to months) of weakness affecting the ability to climb stairs, carry heavy shopping or get up from a chair.
- Muscle tenderness (myalgia) is present in just 25-50% of patients.
- In Inclusion body myositis, the hand muscles can also be involved

- Skin Rash
- Seen in Dermatomyositis
- Red/pink rash
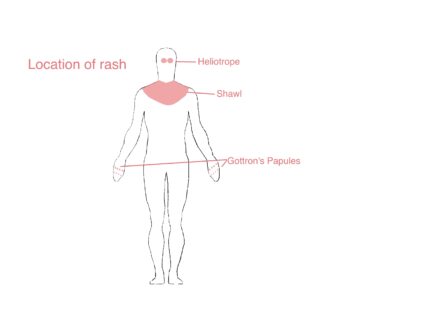
- Upper eyelids (Heliotrope rash)
- Face (erythema)
- Backs of the fingers (Gottron’s papules)
- Rash over the shoulders (shawl sign)
- Sometimes the cuticles of the nails appear to be ragged and have small red dots. This is the result of changes to the small nail fold blood vessels (called capillaries)
- ‘Mechanics hands’-in anti-synthetase syndrome, thickened, fissured skin forms over the fingers on the palmar side of the hand.
- Other muscle involvement
- The oesophagus (gullet) leading to weakness when swallowing food. This can lead to food feeling like it is ‘sticking’ (dysphagia) or to aspiration of food/liquid into the windpipe (trachea).
- The heart muscle can also rarely to affected too.
- The diaphragm can be involved, leading to shortness of breath.
- Complications
- Anti-synthetase syndrome
- Clinically different subset consisting of myositis, arthritis and lung disease
- Lungs
- Interstitial lung disease (ILD)- scarring and fibrosis can cause a chronic cough and shortness of breath
- If ILD progresses it can put strain on the right side of the heart, called pulmonary hypertension and subsequently lead to heart failure.
- Heart
- Abnormal heart rhythms can occur. Risk of heart attacks is slightly increased.
- Cancer
- There is a small increased risk of developing cancer, particularly with dermatomyositis.
How do we diagnose Idiopathic Inflammatory Myopathies?
Diagnosis is based on the symptoms, examination and investigations carried out. The assessment of muscle strength will be closely examined.
It is important to rule out any other conditions that could mimic the same symptoms.
Investigations include:
- Blood tests:
- General- Full blood counts, liver and kidney function
- Inflammatory markers- ESR and CRP
- Muscle enzyme- Creatine Kinase (CK)- usually raised
- Thyroid function tests
- Autoantibody tests- ANA, ENA and myositis-specific autoantibodies
- Electromyography (EMG)
- A needle electrode is inserted into the affected muscles and records the electrical patterns causing movements in your muscles
- MRI scans
- MRI scans can show which muscles are inflamed. This is often used before a biopsy is taken
- Muscle biopsy
- Sending a sample of the affected muscle to the laboratory can help diagnosis by specific tests carried out by a pathologist.
- Lung assessments
- Chest X-rays and CT scans are used along breathing tests called pulmonary function tests
- Heart assessments
- ECG heart tracing and echocardiograms are used
Treatment
- Drug therapies
- Steroids, such as prednisolone are given in high doses initially.
- DMARDs are often introduced to help reduce the steroid doses quicker and avoid side effects
- Occasionally other medications such as biological therapy or immunoglobulins are used.
- Graded exercise programme
- Under a physiotherapist
- Helps restore muscle strength and improve stamina.
Regular monitoring of muscle strength and blood CK will be used to ensure the myositis is under good control.
Useful Links
Versus Arthritis: http://www.versusarthritis.org
Myositis UK: https://www.myositis.org.uk
NHS: https://www.nhs.uk/conditions/myositis/

