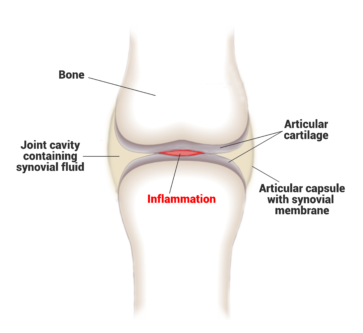
Rheumatoid arthritis (RA) is a chronic inflammatory disease that can affect joints that have a ‘synovial lining’. The synovial lining of a joint is a special layer of cells that protects the joint and secretes lubricants to help the joint to move smoothly.
Inflammation is a response of the body to injury or infection. It is driven by the immune system. In RA, cells from the immune system migrate to joints and become activated, which leads to inflammation and eventually joint damage. As the immune system cells appear to target healthy tissue, RA is known as an autoimmune disease. It is the commonest autoimmune arthritis.
Around 400,000 adults in the UK have rheumatoid arthritis (RA), with 20,000 new cases in the UK every year.
Although the cause of RA remains unknown, inherited (genetic) and environmental factors have been identified as risk factors for developing the disease.
Redness of the joint is not a sign of RA and should be assumed to be infection that needs urgent review by a doctor.
Blood tests:
Imaging
Early referral and prompt treatment as soon as possible after symptoms have started has been shown to lead to the best long-term outcome. Although there is currently no cure for RA, current treatments can lead to low disease activity in the majority of patients.
The mainstay of treatment with Disease-modifying anti-rheumatic drugs (DMARDs).
The most commonly prescribed DMARDs are:
They can be given separately or as a combination. They can take up to 12 weeks to have effect and may require dose adjustments.
Studies have shown that a short course of oral steroids taken at the time of diagnosis along with the DMARDs described above will not only lead to rapid and total resolution of joint inflammation whilst the DMARDs take effect, but will also help to prevent long term damage to joints five years later. [1]
At other times during acute flares of the joints we often prescribe either an intramuscular injection of steroids or steroid joint injections.
Drugs such as painkillers may also be prescribed to help reduce the pain. They include non-steroidal anti-inflammatory drugs (NSAIDs) like ibuprofen. These are good for relieving symptoms but have no effect on progression of the disease. NSAIDs should not be taken at the same time as steroid therapy. NSAIDs can be detrimental to both the kidneys and bowels so for RA we tend to use them in short courses rather than for long periods of time.
Biological DMARDs are prescribed as second line therapy if synthetic DMARDs fail to control inflammation and if the inflammation score is above a certain threshold.
Further information on drug management can be found in the Drugs section of the website.
Assessment of disease activity
To ensure that the treatments are working, we usually monitor your joints in our clinics to assess activity.
In RA this is done by a joint examination of the number of tender and swollen joints and used with your blood inflammation markers and your assessment of how active you feel your arthritis has been in the last week, to calculate a score. The most common score used is a DAS 28.
Click here for a link to the assessments
Versus Arthritis: http://www.versusarthritis.org
NRAS: http://www.nras.org.uk
[1] Landewé RB, Boers M, Verhoeven AC, Westhovens R, van de Laar MA, Markusse HM, van Denderen JC, Westedt ML, Peeters AJ, Dijkmans BA, Jacobs P, Boonen A, van der Heijde DM, van der Linden S. COBRA combination therapy in patients with early rheumatoid arthritis: long-term structural benefits of a brief intervention. Arthritis Rheum. 2002 Feb;46(2):347-56. doi: 10.1002/art.10083. PMID: 11840436.